Suicide Data on Children as Young as 10 Review
- Review
- Open Access
- Published:
Registered psychiatric service use, cocky-damage and suicides of children and young people anile 0–24 earlier and during the COVID-xix pandemic: a systematic review
Child and Adolescent Psychiatry and Mental Health volume 16, Article number:15 (2022) Cite this article
Abstruse
Background
The COVID-19 pandemic has impacted on psychiatric symptoms of children and young people, just many psychiatric services accept been disrupted. Information technology is unclear how service apply, cocky-impairment and suicide has inverse since the pandemic started. To gain timely data, this systematic review focused on studies based on authoritative data that compared psychiatric service use, self-harm and suicide earlier and during the pandemic among children and young people.
Methods and finding
A systematic review of studies published in English from 1 January 2020 to 22 March 2021 was conducted, using the Spider web of Scientific discipline, PubMed, Embase and PsycINFO databases. Increases or reductions in service use were calculated and compared using percentages. Of the 2,676 papers retrieved, eighteen were eligible for the review and they provided information from xix countries and regions. Most studies assessed changes during the early on phase of the COVID-nineteen pandemic, from March to July 2020, and three assessed the changes until Oct 2020. Fifteen studies reported a total of 21 service utilize outcomes that were quantitively examined. More than three-quarters of the 21 outcomes (81%) fell by 5–80% (mean reduction = 27.nine%, SD = 35%). Ten of the twenty outcomes for psychiatric emergency department (ED) services reduced by 5% to eighty% (mean = forty.1%, SD = 34.9%) during the pandemic. Reductions in service use were also recorded for ED visits due to suicide ideation and self-harm, referrals to secondary mental wellness services, psychiatric inpatient unit of measurement admissions and patients receiving handling for eating disorders. Withal, in that location were also some increases. Suicide rate and the number of ED visits due to suicide attempts have increased, and there was an increase in the number of treatment sessions in a service that provided telemedicine.
Conclusion
Virtually of the studies showed reductions in the use of psychiatric services by children and immature people during the early on phase of the pandemic and this highlighted potential delays or unmet needs. Suicide rate has increased during the second moving ridge of the pandemic. Further studies are needed to appraise the pattern of service use in the afterwards phases of the COVID-19 pandemic.
Background
The COVID-xix pandemic has affected the health of individuals and the means that healthcare systems work. Mandatory lockdowns and quarantine periods, schoolhouse closures and social restrictions have been effective in mitigating the spread of the virus, but these measures have probably increased psychiatric symptoms among children and young people. Emerging evidence suggests that psychiatric symptoms take worsened among children and immature people across the globe during the COVID-19 pandemic, deteriorating their level of mental health [1,2,3]. There have also been reports of increased suicides in this historic period range during the second wave of the pandemic, in the third quarter of 2020 [4]. COVID-nineteen restrictions meant that psychiatric services were close downwardly, or restricted, and the general use of psychiatric services has decreased [5,6,7]. Systematic information near how services take been used by children and young people with mental health problems during the pandemic is imperative. This will help united states to program electric current services more than effectively and mitigate the effects of the current and future phases of the pandemic.
A contempo systematic review investigated the global bear upon that the COVID-19 pandemic has had on how the general population take used broader healthcare services, including visits, admissions, diagnostics and therapeutics [viii]. It reported that the utilise of healthcare services had fallen past a third for various outcomes, mainly those related to physical health [eight]. Withal, the review did not nowadays psychiatric services separately and cleaved down past dissimilar age groups. Empirical studies of full general populations have reported decreases in primary care psychiatric services [v, half dozen] and reduced referrals to secondary care psychiatric services [7]. A large-scale survey of psychiatrists across Europe reported a meaning subtract in mental health services during the get-go wave of the COVID-19 pandemic in 2020 [ix]. The use of psychiatric services by children and young people has constantly increased over the last 3 decades [10,xi,12,13,14,xv,xvi]. However, we are non aware of whatsoever systematic reviews that have specifically focused on registered psychiatric service utilise, self-harm and suicide by children and immature people before and during the COVID-19 pandemic.
That is why this systematic review was both timely and needed. We focused on studies that used administrative data as it can provide large datasets in a timely manner. Authoritative data tin also requite reliable data of the trends of psychiatric service use and rare events such as suicide deaths. This systematic review aimed to evaluate the existing literature on registered psychiatric services, self-harm and suicides for children and young people anile 0–24 years of age, before and during the COVID-nineteen pandemic. We too wanted to specifically focus on how the use of different services had inverse.
Methods
Search strategy and option criteria
This systematic review was conducted in accordance with the Preferred Reporting Items of Systematic Reviews and Meta-analyses (PRISMA) [17]. The review protocol was prospectively registered with the International Prospective Register of Systematic Reviews (PROSPERO registration number CRD42021238999). Comprehensive searches of electronic databases were carried out and these focused on potentially relevant studies that were published in English language between ane Jan 2020 and 22 March 2021. The databases that were searched were: Web of Science, PubMed, Embase and PsycINFO. Potential papers were likewise identified using hand searches and the backward snowballing technique [xviii], which involves looking at the reference lists of the selected papers. All titles identified for screening were exported to the Mendeley reference director program. The search and screening processes were conducted past 2 reviewers (Wan Mohd Azam Wan Mohd Yunus; AY and Laura Kauhanen; LK). They independently screened the papers based on the titles and abstracts afterwards removing whatsoever duplicates. Any disagreements were discussed with two senior researchers; an banana professor and a professor (David Gyllenberg; DG and Andre Sourander; Equally). Then the two reviewers (AY and LK) independently conducted full-text assessments based on the predefined inclusion and exclusion criteria. Both of the reviewers cross-checked the included papers and whatever disagreements were discussed and resolved with the 2 senior researchers. The total search terms are included in the Additional file 1: Appendix 1.
Inclusion and exclusion criteria
Studies on services use, cocky-harm and suicide deaths of children and young people from 0–24 years of age were included. The World Health Organisation (WHO) definition of young people (10–24 years) were used. Immature people too fitted well with the menses of 'boyhood' defined past Sawyer et al. [19], which was as well 10–24 years. Studies that included singled-out sub-samples of individuals anile 0–24 were included. We considered any studies that used clinical, register-based, hospital or health organisation administrative data, medical records or national records that reported psychiatric service utilize, self-impairment and/or suicides data before and during the pandemic. The 'before and during the pandemic' period was defined equally any menstruum during the COVID-19 pandemic and at least 1 corresponding period in the years before the pandemic, equally defined by the authors of the studies that were included. Only scientific peer-reviewed papers that were published in English were considered. Any psychiatric service utilise outcomes earlier and during the COVID-19 pandemic periods were included, such every bit referrals, visits and presentations, admissions, diagnostics or therapeutic services.
Quality assessment
The quality of the studies were assessed using the National Institutes for Health Study Quality Cess Tool for Observational Accomplice and Cross-Sectional Studies [20]. The tool comprised 14 items that assessed the potential take chances of selection bias, information bias, measurement bias, confounding bias, report ability and the strength of the causality in the associations between the exposure and outcomes. Two reviewers (AY and LK) divided the studies in half and rated each report independently. They so rated the other half and compared the coding for agreement. Disagreements were resolved through discussions with a third reviewer (DG).
Information extraction and synthesis
The following data were extracted from the included studies into an Excel spreadsheet: writer, country, source of the data, historic period, earlier and during pandemic timeframes, any data before and during the pandemic timepoints, outcomes and key findings. Any descriptive data on the frequencies, ways and percentages of the outcomes were extracted, where available. The percentage changes before and during the COVID-19 pandemic were calculated using relative service utilise changes, as used in other studies [21,22,23,24]. If the assessed outcomes were available in at least five studies, nosotros quantified the crude ways, standard deviations (SD) and ranges of the changes across the studies. Due to considerable heterogeneity in the blueprint and outcomes of the included studies, we refrained from weighting results based on factors such equally sample size. Where bachelor, statistical non-significance was included as reported past the original papers. A narrative synthesis was used to synthesize all the other findings.
Results
Study selection and retrieval procedure
The initial database and manual searches identified 2676 citations and 575 duplicates were removed. The titles and abstracts of the other 2101 records were screened for eligibility, 1969 records were excluded and the total texts of 132 papers were evaluated. We excluded 114 full texts because they did non provide any timepoints to specify the periods before and during COVID-19, they did not provide whatsoever specific data or interpretation for individuals aged 0–24 or they did non focus on psychiatric service use, self-harm or suicide. At the end of this process, 18 studies were included in the qualitative synthesis. Figure 1 displays the PRISMA flow diagram for the screening and study choice processes.
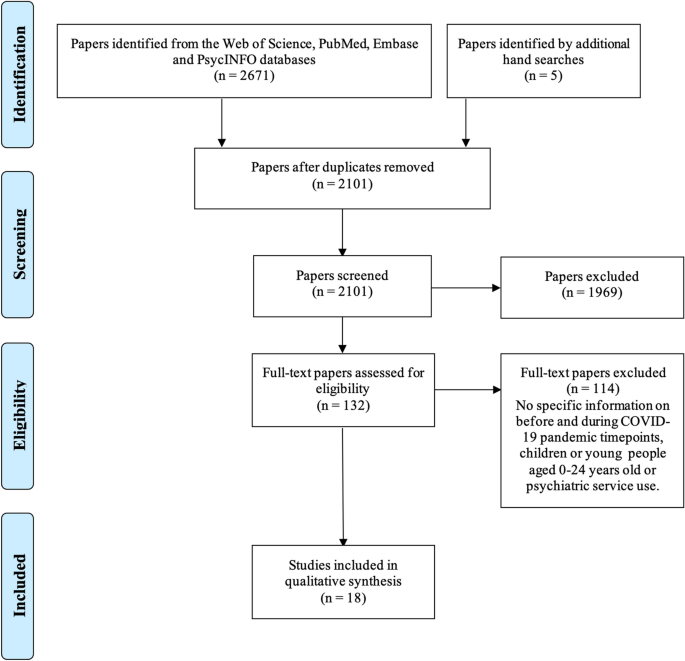
PRISMA flow diagram on how the papers were selected for the review
Characteristics of the included studies
Countries covered by the studies
Information from 19 countries and regions were included. There were 17 studies that focused on merely one country and these were all conducted in developed countries: six were from the Usa [22, 24,25,26,27,28], two from the United kingdom [7, 29], ii from Nihon [4, 30], and one each from Spain [31], Italy [23], New Zealand [32], Commonwealth of australia [21], Canada [33], France [34] and Israel [35]. The other written report comprised data from 10 different countries and regions: England, Scotland, Ireland, Austria, Italy, Hungary, Serbia, Turkey, Oman, and the United Arab Emirates [36].
Timepoints for measuring registered data
Figure 2 shows the time windows when psychiatric service utilise, cocky-harm or suicide data was measured earlier and during the COVID-19 pandemic. Most of the studies assessed the early phase of the health emergency, which was declared a pandemic by the WHO on 11 March 2020, and 15 of the studies extended the follow-up period until April to July 2020. Iii studies monitored service utilize upwardly to Oct 2020. The definition of the before and during pandemic periods varied widely betwixt the studies. Most compared information during a COVID-nineteen period in 2020 and one previous year [7, 21,22,23, 25, 26, 28, 31, 33, 34, 36] and 5 used more than one previous yr [4, 24, 27, thirty, 35]. The other 2 used an before pre-pandemic timepoint in 2020 [29, 32]. Based on the information available in each newspaper, majority of the included studies defined the start of the pandemic period as the date when the primeval restrictions were imposed or each location went into lockdown. This tended to be the finish of February to mid-March 2020, as depicted by the yellow lines in Fig. 2.

Timeframes covered by the data before (blue) and during (grey) the COVID-19 pandemic.The xanthous lines describe the showtime lockdowns or restrictions, based on information from the study authors. a,b,c,d,eastwardBefore pandemic timeframe started earlier January 2019: a March to May 2018 and 2019, b January to December 2010–2019, c 7 March to six May 2018 and 2019, dNovember 2016 to Jan 2020, eJanuary to October 2015–2019
Quality assessment
It was notable that 12 of the xviii studies did not appraise any potential confounding variables in their analyses. We defined these every bit seasonal trends or demographic differences that could be statistically measured and adjusted for in order to mitigate confounding bias. Despite this, all 18 studies were included in the review, every bit they were all explanatory in nature and collected data from electronic, administrative or national records. The summary of the 14 quality cess items is in the Additional file 2: Appendix 2.
Changes before and during the COVID-19 pandemic
The key findings for each study are shown in Table 1 and Fig. 3 summarises the percentage changes for the different service use outcomes. The percentage changes are illustrated using dotted chart. The y-axis represents the service use outcomes and the x-axis is the percentage change before and during the COVID-19 pandemic. Positive percentage changes signify an increase, while negative pct alter bespeak a reduction in service use, recorded by each study for that detail outcome. All except iii [4, 27, 30] of the 18 studies provided descriptive data for standardized comparisons. Another written report conducted at a unmarried paediatric emergency section (ED) in New York was excluded from the quantitative analysis because information technology combined iii different outcomes as one, namely ED visits due to suicide ideation, self-impairment and suicide attempts [24]. In our review these outcomes were assessed separately. Eight studies reported more than 1 outcome [23,24,25, 29, 31, 32, 35, 36] and this meant that a full of 21 outcomes were assessed. The changes in the service utilize of these 21 outcomes ranged from a reduction of 80% to an increase of 48.i%, with a crude mean change of − 27.9% and a standard deviation (SD) of 35%.
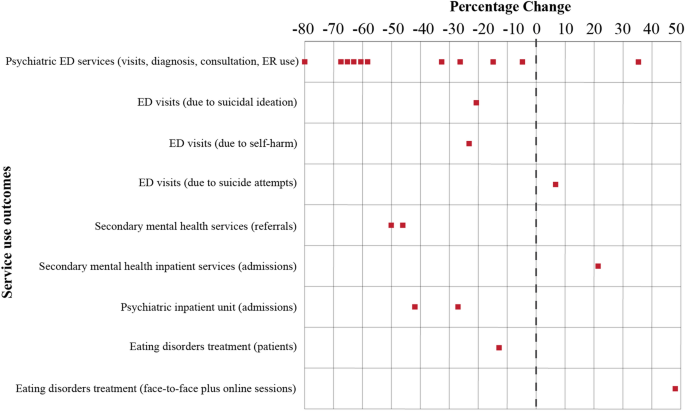
Percentage of service use changes before and during the COVID-19 pandemic. Crimson dots refer to percentage changes recorded by one written report for one detail outcome
Of the fourteen studies, 11 had at least 1 outcome related to ED services, including the number of psychiatric visits or presentations, ED employ, diagnoses and consultations. Only one written report recorded an increase in psychiatric visits to the ED, of 35.3% [21], while the other studies recorded reductions of between 5.i and fourscore.0% [22,23,24, 26, 28, 31, 32, 34, 36]. The average percentage change was 40.ane ± 34.9% in psychiatric ED services during the COVID-xix pandemic when the data were compared to before the pandemic.
Two studies reported changes ED visits due to suicide ideation, cocky-harm and/or suicide attempts while two studies in Japan reported data on the suicide rates based on nationwide records. 1 report reported a reduction in total ED visits due to suicide ideation (20.vii%), but a slight increment in visits due to suicide attempts (half-dozen.7%) [25]. However, the authors concluded that the rates of suicide ideation were not uniformly higher past month, from January to July 2020, compared to the same menses in 2019. Despite the reduction in total ED visits due to suicide ideation in January to July 2020, compared to the same menses in 2019, the charge per unit of suicidal ideation was one.half-dozen times higher in March 2020 and one.45 times college in July 2020. This report besides reported that the rates of suicide attempts were between 58 and 134% higher in Feb, March, April and July 2020, compared to the same months in 2019. Information technology too reported that suicide ideation was more frequent among females in 2020 than 2019 [25]. Some other study conducted in ten different countries and regions reported a 23.two% reduction in pooled ED visits due to self-harm [36]. However, a more than detailed analysis by that report showed that the number of children and young people who presented with self-harm, every bit a percentage of total psychiatric ED visits, increased from 50% in 2019 to 57% in 2020, with area-specific increases in x of the 14 areas covered by the 10 countries. Their study also found higher proportions of children and young people who had previously visited hospitals subsequently self-harming (36% in 2020 versus 29% in 2019) or had self-harmed in the community (71% in 2020 versus 63% in 2019). One of the study conducted in Nippon during the initial phase (March to May 2020) of the pandemic reported no statistically significant difference of suicide rates among children and adolescents [30]. Nonetheless some other contempo study also in Nippon with more comprehensive data reported that the suicide rate amongst children and adolescents has increased 49% in the 2nd wave (July to October 2020) of the pandemic [4].
Two studies from the UK reported reductions in referrals to secondary mental health services of 43.i% [seven] and l.7% [29]. In contrast, secondary mental health inpatient services admissions had increased by 21.4%, but the increase was not statistically pregnant [29]. Two studies reported that the number of patients admitted to psychiatric acute inpatient units fell by 27.0% [36] and 41.ix% [31]. The 2nd study also reported a reduction in the average infirmary length of stay, from fourteen.32 ± 10.23 to eight.94 ± 4.87 days (p = 0.08).
Ane report from State of israel focused on a handling eye for eating disorders. The authors reported that the number of patients reduced past 12.eight%, merely the number of treatment sessions increased by most half (48.1%) during the pandemic [33]. The authors added that the treatment centre had moved from just face-to-face sessions before the pandemic to a combination of face-to-face and online sessions during the pandemic. This explained the increased number of sessions during the pandemic.
Discussion
Our systematic review identified eighteen studies from 19 countries and regions that focused on diverse psychiatric service use, self-harm and suicide of children and immature people during the COVID-19 pandemic. These were compared to various periods earlier the pandemic. The principal finding was that there were reductions in the use of psychiatric services past children and young people. The most striking reductions related to ED services during the early phase of the COVID-nineteen pandemic. Secondly, suicide rates accept increased during the second wave of the pandemic, based on the nationwide records study in Japan. Limited evidence suggested that ED visits due to suicide ideation and self-harm reduced, but visits due to suicide attempts increased amongst children and immature people during the early COVID-19 pandemic. These findings provide essential information that tin can help us to plan adequate psychiatric services for children and immature people during whatever future pandemics or crises.
Our review extends the findings of a broad systematic review on the disruptive global impact of the COVID-19 pandemic on healthcare services [8]. Information technology demonstrates how children and immature people accessed fewer psychiatric services during the COVID-19 pandemic than earlier the pandemic. A number of healthcare services were reduced during the early on stage of the COVID-19 pandemic. Healthcare services are considered essential services, but a WHO survey carried out in summertime 2020 reported that only one-half of the countries in its member states ensured the continuity of services for mental, neurological and substance use disorders in their national COVID-19 response programmes [37]. These approaches may have also disrupted the continuity of psychiatric services. Most of the pandemic data collected by the studies we reviewed focused on when restrictions had simply been imposed in the corresponding countries. More inquiry is needed to show the furnishings of more extended restrictions.
We consider the perceived benefits versus risks as the possible primary explanation for the findings, particularly the reduction of ED visits. In the early phase of the pandemic, authorities continuously emphasized and broadly publicized the need to stay at habitation, and only leave the firm when necessary. This may have afflicted the motivation of children and young people to access psychiatric services. Parents and adolescents might perceive that the clear and quick benefit of keeping themselves, their family unit and their children safe at home outweighs the risks to leave and access ED services for acute psychiatric-related bug unless for severe cases. The pandemic has had a number of negative impacts on diverse aspects on people's lives, including endmost schools and public places, changes in work routines and how companies operate and how families have had to organize their daily lives. This forced isolation has led to feelings of helplessness, abandonment and heightened insecurity [38]. Public health measures, such as concrete distancing and quarantine periods to reduce the spread of the coronavirus, may have also reduced emergency department visits and this has meant that less children and adolescents have sought help for physical and mental wellness atmospheric condition [39,twoscore,41]. Fear of contracting the virus [38] could have played a primal role in reduced healthcare visits and there are two possible pathways when it comes to children and young people. The first is negative data from teachers, peers or social media and the 2d is modelling, whereby individuals are influenced by the fear that their parents feel [42]. This has probably led to increased unmet needs amid children and immature people and delayed help-seeking, which poses capacity challenges for psychiatric services. Some psychiatric disorders can exist aggravated without timely intervention and experiencing psychiatric problems during sure periods of development may predict long-term adverse outcomes [43, 44].
We likewise identified a report that showed how psychiatric services adjusted to the pandemic. For example, i study reported that the unprecedented utilise of multi-professional person telemedicine treatment sessions enabled them to maintain the continuity of eating disorder treatment sessions, by adding another mode of delivery to face-to-confront sessions [35]. That report found that, although the average number of patients receiving treatment had fallen in 2020, compared to the average same periods from 2015 to 2019, the combined number of face-to-face up plus telemedicine sessions had increased considerably (48.1%) during the COVID-19 pandemic. This ability to accommodate during a public health crunch provides a glimpse of the vast potential that technological advances tin can offer when it comes to transforming the delivery of sure traditional psychiatric services. This increase may signpost the way to improving the toll-effectiveness of future treatment and inquiry is needed to show how this tin be sustained in the longer term. These findings back up arguments that the COVID-19 pandemic has been described as an unpredictable 'blackness swan moment' [45]. One article stated that it will lead to a 'partly, though robust, shift in mental health intendance provision towards online prevention, treatment, and care in the near future' [46].
Service apply changes related to suicide ideation, cocky-damage and/or suicide attempts were only covered past ii studies [25, 36] and there were two studies on nationwide suicide deaths record in Nippon [four, 30]. Several findings can be fatigued from these studies. The multinational written report of 10 countries and regions by Ougrin et al. reported a reduction in the bodily number of ED visits due to self-harm. However, a more than detailed analysis of the pooled information showed that self-impairment accounted for a slightly college proportion of psychiatric ED visits, increasing from 50% in 2019 to 57% in 2020 [36]. Colina et al. [25] reported a similar blueprint. Despite the lower number of total ED visits due to suicidal ideation from January to July 2020, compared to 2019, the by-month analysis showed no uniform pattern. However, a higher rate was seen in March 2020, which corresponded to the early on COVID-xix measures and the WHO declaring the outbreak a pandemic. While the total number of ED visits due to suicide attempts slightly increased, the rates were significantly higher in Feb, March, April and July 2020 when they were compared with the same months in 2019 [25]. Information technology should exist emphasised that these total numbers only represented the number of children and young people who went to the ED. Nigh young people with suicidal ideation and self-harm exercise not seek professional help and are more probable to seek informal aid from their peers [47]. COVID-19 may have restricted social interaction with peers and reluctance to seek assist from healthcare facilities, considering of the fear of infection [38], may explain the reductions in ED visits. These information betoken to unmet needs, rather than bodily reductions in needs. Previous reviews take highlighted suicidal ideation and prior attempts as major risk factors for suicide in children [48] and young people [49]. Notably, a Japanese report that was based on national statistics reported increases in suicide rates by age. It found that the rate was highest in those anile below twenty years (49%) during the 2nd wave of the COVID-19 pandemic, compared to other age groups [iv]. This could signify a worrying indicator and calls for immediate interventions to tackle suicidality in children and young people.
Strengths and limitations
To our knowledge, this is the first systematic review to collate empirical prove of the changes in registered psychiatric service use, self-harm and suicide deaths among children and immature people anile 0–24 during the early stages of the COVID-19 pandemic, compared to earlier the pandemic. The review followed rigorous PRISMA guidelines. We also quantified the changes by presenting them as percentages and that allowed u.s. to brand standardized comparisons betwixt the diverse service use outcomes in the selected studies beyond different countries. These findings are imperative at a time when children, young people and health intendance services go along to adapt to the ambiguities acquired past the COVID-xix pandemic. This review had a number of limitations. First, merely peer-reviewed papers published in English were searched for and included, which meant that potential studies in other languages and papers that had not been peer-reviewed were not included. 2nd, although eighteen studies were included in the review, children and immature people and psychiatric services were subgroups in xi of those studies. In those cases, we just extracted the data pertaining to the use of psychiatric services by children and immature people anile 0–24 years old and this did limit our interpretations of these studies. 3rd, 13 of the18 studies express the before and during pandemic periods to only 2020 and 2019. Fourth, we identified express evidence on service use outcomes beyond ED visits or presentations. In item, only a express number of studies assessed the post-obit outcomes: admission to secondary mental health services, psychiatric inpatient unit of measurement admissions, diagnoses and consultations and the number of patients who received psychiatric treatment sessions and how many they required. In addition, our review merely identified one study that assessed how psychotherapeutic services were used to address mental health and psychiatric issues and that was express to merely eating disorders [35]. Fifth, 17 of the 18 studies were conducted in high-income countries, based on the World Bank listing. The exception was the multinational study that included data from Serbia and Turkey, which are ii center-income countries [36]. No studies included in our review that were conducted in depression-income countries.
Conclusion
This systematic review showed a considerable reduction in the use of psychiatric service utilize by children and young people aged 0–24 during the initial phase of the COVID-19 pandemic, compared to before the pandemic. This was despite emerging evidence that psychiatric symptoms seemed to increase among children and young people, signifying possible unmet needs or delayed access to psychiatric services. Many countries observed this design for dissimilar psychiatric service use outcomes. Our findings have three public health significance. First, the COVID-19 pandemic highlighted the need for active plans on reassuring children'southward and young people'south admission to services as the current pandemic proceeds and future pandemics and crises are possible. Second, the pandemic has challenged traditional contiguous services, but it has likewise highlighted the potential of integrating technological advances into psychiatric services. Third, changes in the way that children and young people use services may as well modify traditional help-seeking models. Further research is needed on how to improve the efficient utilize of psychiatric services amidst children and young people and how these services can be maintained.
Availability of data and materials
Not applicative.
References
-
Meherali South, Punjani Due north, Louie-Poon S, Abdul Rahim K, Das JK, Salam RA, et al. Mental health of children and adolescents amidst CoViD-nineteen and by pandemics: a rapid systematic review. Int J Environ Res Public Wellness. 2021;xviii(seven):3432.
-
Racine N, McArthur BA, Cooke JE, Eirich R, Zhu J, Madigan S. Global prevalence of depressive and feet symptoms in children and adolescents during COVID-19: A meta-assay. JAMA Pediatr. 2021;175:1142.
-
Samji H, Wu J, Ladak A, Vossen C, Stewart E, Pigeon N, et al. Mental health impacts of the COVID‐19 pandemic on children and youth–a systematic review. Kid Adolesc Mental Health. 2021.
-
Tanaka T, Okamoto Due south. Increase in suicide post-obit an initial decline during the COVID-19 pandemic in Japan. Nature Hum Behav. 2021;5(two):229.
-
Mansfield KE, Mathur R, Tazare J, Henderson AD, Mulick AR, Carreira H, et al. Indirect acute effects of the COVID-nineteen pandemic on concrete and mental health in the United kingdom: a population-based study. Lancet Digital Health. 2021;3(4):e217–30.
-
Williams R, Jenkins DA, Ashcroft DM, Brown B, Campbell S, Carr MJ, et al. Diagnosis of concrete and mental health weather in chief care during the COVID-xix pandemic: a retrospective cohort study. Lancet Public Health. 2020;5(10):e543–50.
-
Chen S, She R, Qin P, Kershenbaum A, Fernandez-Egea Due east, Nelder JR, et al. The medium-term impact of COVID-19 lockdown on referrals to secondary care mental health services: a controlled interrupted time series report. Forepart Psychiatry. 2020;11:1307.
-
Moynihan R, Sanders S, Michaleff ZA, Scott AM, Clark J, To EJ, et al. Impact of COVID-19 pandemic on utilisation of healthcare services: a systematic review. BMJ Open up. 2021;xi(iii):e045343.
-
Rojnic Kuzman M, Vahip S, Fiorillo A, Beezhold J, Pinto da Costa M, Skugarevsky O, et al. Mental health services during the first wave of the COVID-19 pandemic in Europe: results from the EPA Ambassadors Survey and implications for clinical exercise. Eur Psychiatry. 2021;64(1):e41.
-
Lempinen L, Luntamo T, Sourander A. Changes in mental health service use among viii-year-old children: a 24-twelvemonth time-trend study. Eur Child Adolesc Psychiatry. 2019;28(iv):521–30.
-
Sourander A, Lempinen L, Brunstein KA. Changes in mental health, bullying beliefs, and service use among eight-yr-old children over 24 years. J Am Acad Child Adolesc Psychiatry. 2016;55(8):717-25.e2.
-
Gyllenberg D, Marttila Grand, Sund R, Jokiranta-Olkoniemi E, Sourander A, Gissler M, et al. Temporal changes in the incidence of treated psychiatric and neurodevelopmental disorders during adolescence: an analysis of two national Finnish birth cohorts. Lancet Psychiatry. 2018;5(3):227–36.
-
Gyllenberg D, Gissler M, Malm H, Artama M, Hinkka-Yli-Salomäki S, Brown As, et al. Specialized service utilize for psychiatric and neurodevelopmental disorders by age 14 in Finland. Psychiatr Serv. 2014;65(3):367–73.
-
Atladottir HO, Gyllenberg D, Langridge A, Sandin South, Hansen SN, Leonard H, et al. The increasing prevalence of reported diagnoses of childhood psychiatric disorders: a descriptive multinational comparison. Eur Child Adolesc Psychiatry. 2015;24(2):173–83.
-
Potrebny T, Wiium Due north, Haugstvedt A, Sollesnes R, Wold B, Thuen F. Trends in the utilization of youth primary healthcare services and psychological distress. BMC Health Serv Res. 2021;21(1):115.
-
Mojtabai R, Olfson M. National trends in mental health treat US adolescents. JAMA Psychiat. 2020;77(seven):703–14.
-
Moher D, Liberati A, Tetzlaff J, Altman DG. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. BMJ. 2009;339:b2535.
-
Wohlin C. Guidelines for snowballing in systematic literature studies and a replication in software engineering. In: Proceedings of the 18th international briefing on evaluation and cess in software engineering, London, England, United Kingdom: Association for Computing Machinery; 2014. p. Article 38.
-
Sawyer SM, Azzopardi PS, Wickremarathne D, Patton GC. The historic period of adolescence. Lancet Kid Adolesc Health. 2018;2(three):223–viii.
-
National Institutes for Health. Study quality assessment tool for observational cohort and cantankerous-sectional studies 2021. http://www.nhlbi.nih.gov/health-topics/study-quality-assessment-tools.
-
Cheek JA, Craig SS, Westward A, Lewena Southward, Hiscock H. Emergency section utilisation by vulnerable paediatric populations during the COVID-xix pandemic. Emerg Med Australas. 2020;32(5):870–1.
-
Leff RA, Setzer E, Cicero MX, Auerbach M. Changes in pediatric emergency department visits for mental health during the COVID-19 pandemic: a cross-sectional study. Clin Child Psychol Psychiatry. 2021;26(i):33–8.
-
Raucci U, Musolino AM, Di Lallo D, Piga S, Barbieri MA, Pisani Thou, et al. Impact of the COVID-19 pandemic on the Emergency Department of a third children's hospital. Ital J Pediatr. 2021;47(1):ane–12.
-
Sokoloff WC, Krief WI, Giusto KA, Mohaimin T, Murphy-Hockett C, Rocker J, et al. Pediatric emergency department utilization during the COVID-19 pandemic in New York City. Am J Emerg Med. 2021;45:100–4.
-
Colina RM, Rufino Thousand, Kurian Due south, Saxena J, Saxena One thousand, Williams L. Suicide ideation and attempts in a pediatric emergency section before and during COVID-19. Pediatrics. 2021;147(3):e2020029280.
-
Levene R, Fein DM, Silver EJ, Joels JR, Khine H. The ongoing impact of COVID-nineteen on asthma and pediatric emergency health-seeking behavior in the Bronx, an epicenter. Am J Emerg Med. 2021;43:109–xiv.
-
Pelletier JH, Rakkar J, Au AK, Fuhrman D, Clark RSB, Horvat CM. Trends in US pediatric hospital admissions in 2020 compared with the decade before the COVID-19 pandemic. JAMA Netw Open. 2021;4(2):e2037227.
-
Leeb RT, Bitsko RH, Radhakrishnan L, Martinez P, Njai R, Holland KM. Mental wellness-related emergency department visits amid children aged <xviii years during the COVID-19 pandemic—United States, January 1-Oct 17, 2020. MMWR Morb Mortal Wkly Rep. 2020;69(45):1675–lxxx.
-
Tromans Southward, Chester Five, Harrison H, Pankhania P, Booth H, Chakraborty N. Patterns of use of secondary mental wellness services before and during COVID-nineteen lockdown: observational written report. Bjpsych Open up. 2020. https://doi.org/ten.1192/bjo.2020.104.
-
Isumi A, Doi S, Yamaoka Y, Takahashi K, Fujiwara T. Do suicide rates in children and adolescents change during school closure in Japan? The acute effect of the first wave of COVID-19 pandemic on child and adolescent mental wellness. Child Abuse & Neglect. 2020;110(Part 2):104680.
-
Díaz de Neira M, Blasco-Fontecilla H, García Murillo L, Pérez-Balaguer A, Mallol L, Forti A, et al. Demand analysis of a psychiatric emergency room and an adolescent acute inpatient unit in the context of the COVID-19 pandemic in Madrid, Espana. Forepart Psychiatry. 2020;xi:1533.
-
Bothara RK, Raina A, Carne B, Walls T, McCombie A, Ardagh MW, et al. Paediatric presentations to Christchurch Hospital Emergency Department during COVID-19 lockdown. J Paediatr Kid Wellness. 2021;57(half-dozen):877–82.
-
Goldman RD, Grafstein E, Barclay N, Irvine MA, Portales-Casamar E. Paediatric patients seen in 18 emergency departments during the COVID-19 pandemic. Emerg Med J. 2020;37(12):773–7.
-
Pignon B, Gourevitch R, Tebeka Southward, Dubertret C, Cardot H, Dauriac-Le Masson V, et al. Dramatic reduction of psychiatric emergency consultations during lockdown linked to COVID-19 in Paris and suburbs. Psychiatry Clin Neurosci. 2020;74(x):557–9.
-
Yaffa S, Adi EL, Itai P, Marit JM, Doron G, Daniel S. Treatment of eating disorders in adolescents during the COVID-xix pandemic: a case series. J Eat Disord. 2021;9(one):1–11.
-
Ougrin D, Wong BHC, Vaezinejad 1000, Plener PL, Mehdi T, Romaniuk L, et al. Pandemic-related emergency psychiatric presentations for cocky-damage of children and adolescents in 10 countries (PREP-kids): a retrospective international cohort study. Eur Child Adolesc Psychiatry. 2021. https://doi.org/10.1007/s00787-021-01741-6.
-
Globe Health Organization. The affect of COVID-19 on mental, neurological and substance utilize services: results of a rapid assessment. Geneva: Earth Health Organization; 2020. p. 2020.
-
Ornell F, Schuch JB, Sordi AO, Kessler FHP. "Pandemic fear" and COVID-xix: mental wellness burden and strategies. Braz J Psychiatry. 2020;42(3):232–five.
-
Beck Due north, Michel Chiliad, Klingkowski U, Binder E, Kapelari K, Maurer Thou, et al. The COVID-19 pandemic reduced paediatric emergency department visits just did not significantly increment urgent cases. Acta Paediatrica.n/a(due north/a).
-
Cozzi M, Zanchi C, Giangreco M, Rabach I, Calligaris L, Giorgi R, et al. The impact of the COVID-19 lockdown in Italian republic on a paediatric emergency setting. Acta Paediatr. 2020;109(x):2157–nine.
-
Rhedin SA, Ryd Rinder Grand, Hildenwall H, Herlenius E, Hertting O, Luthander J, et al. Reduction in paediatric emergency visits during the COVID-19 pandemic in a region with open preschools and schools. Acta Paediatr. 2021;110(x):2802–4.
-
Radanović A, Micić I, Pavlović S, Krstić K. Don't Call up That Kids Aren't Noticing: Indirect Pathways to Children'south Fearfulness of COVID-19. Front Psychol. 2021;12:531.
-
Gyllenberg D, Sourander A, Niemelä S, Helenius H, Sillanmäki L, Ristkari T, et al. Childhood predictors of utilize and costs of antidepressant medication by historic period 24 years: findings from the Finnish Nationwide 1981 Birth Cohort Report. J Am Acad Child Adolesc Psychiatry. 2011;50(4):406-15.e1.
-
Sourander A, Gyllenberg D, Klomek AB, Sillanmäki L, Ilola A-Grand, Kumpulainen K. Association of bullying behavior at viii years of age and use of specialized services for psychiatric disorders by 29 years of age. JAMA Psychiat. 2016;73(two):159–65.
-
Blumenstyk G. Why coronavirus looks similar a 'Black Swan' Moment for College Ed: The Chronicle of Higher Education; 2020. https://www.chronicle.com/newsletter/the-border/2020-03-11.
-
Air current TR, Rijkeboer M, Andersson One thousand, Riper H. The COVID-19 pandemic: The 'black swan'for mental health care and a turning point for due east-health. Internet Interv. 2020;xx:100317.
-
Michelmore L, Hindley P. Assist-seeking for suicidal thoughts and self-harm in young people: a systematic review. Suicide Life-Threat Behav. 2012;42(5):507–24.
-
Soole R, Kõlves K, De Leo D. Suicide in children: a systematic review. Arch Suicide Res. 2015;19(three):285–304.
-
McLoughlin AB, Gould MS, Malone KM. Global trends in teenage suicide: 2003–2014. QJM Int J Med. 2015;108(10):765–fourscore.
Acknowledgements
Not applicable.
Funding
This inquiry was funded by the Academy of Finland via a COVID-19 grant (number 335690, PI Gyllenberg) and the INVEST-flagship consortium (number 320162, PI Sourander), and by the Juho Vainio Foundation. The funders had no role in study design, information collection and analysis, determination to publish, or preparation of the manuscript.
Writer information
Affiliations
Contributions
CRediT (Contributor Roles Taxonomy).
Conceptualisation—DG, AS, data curation—AY, LK, DG, Every bit, JB, KB, KM, LL, KP, formal analysis—AY, LK, DG, Every bit, JB, KB, KM, LL, KP, funding acquisition—Equally, DG, investigation—AY, LK, methodology—AY, LK, DG, AS, project administration—DG, AY, LK, supervision—DG, Equally, validation—DG, Equally, visualization—AY, LK, DG, writing—original typhoon—AY, LK, writing—review & editing—AY, LK, DG, Equally, JB, KB, KM, LL, KP, SG, All authors read and approved the final manuscript.
Corresponding writer
Ethics declarations
Ideals approving and consent to participate
Not applicable.
Consent for publication
Non applicable.
Competing interests
The authors declare that they have no competing interests.
Boosted information
Publisher'southward Annotation
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed nether a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, equally long every bit you lot give appropriate credit to the original author(southward) and the source, provide a link to the Creative Commons licence, and bespeak if changes were made. The images or other 3rd party material in this commodity are included in the article's Creative Eatables licence, unless indicated otherwise in a credit line to the material. If textile is not included in the article'south Creative Commons licence and your intended utilize is non permitted past statutory regulation or exceeds the permitted use, you lot will need to obtain permission directly from the copyright holder. To view a re-create of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Eatables Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/one.0/) applies to the data fabricated available in this article, unless otherwise stated in a credit line to the data.
Reprints and Permissions
Near this article
Cite this article
Wan Mohd Yunus, W.Thou.A., Kauhanen, Fifty., Sourander, A. et al. Registered psychiatric service use, self-harm and suicides of children and young people aged 0–24 earlier and during the COVID-19 pandemic: a systematic review. Kid Adolesc Psychiatry Ment Health 16, 15 (2022). https://doi.org/10.1186/s13034-022-00452-three
-
Received:
-
Accepted:
-
Published:
-
DOI : https://doi.org/x.1186/s13034-022-00452-iii
Keywords
- Service use
- COVID-19 pandemic
- Children
- Adolescents
- Young people
- Mental health
- Psychiatric
- Suicide
Source: https://capmh.biomedcentral.com/articles/10.1186/s13034-022-00452-3
0 Response to "Suicide Data on Children as Young as 10 Review"
Post a Comment